10 min read
Don't Get Stressed: How to Find Bill Paying Assistance
Why Financial Stress Shouldn't Mean Losing Your Independence Bill paying assistance is available through government programs, utility providers, and...
8 min read
 Sydney Giffen
:
March 17, 2026
Sydney Giffen
:
March 17, 2026


Fall prevention seniors need to understand starts with three key actions: Move (exercise regularly for strength and balance), Improve (manage medications and health conditions), and Remove (eliminate home hazards). These steps can dramatically reduce fall risk and help older adults maintain their independence at home.
Quick Fall Prevention Checklist:
Falls are the number one reason for injury-related death, hospitalization, and emergency department visits for older adults in Canada. The statistics are sobering: 1 in 3 seniors fall at least once a year, and in Canada, a senior experiences a fall every 12 seconds.
The consequences extend far beyond physical injury. Falls cost the Canadian healthcare system $5.6 billion in 2018 alone—nearly 20% of the total cost of injury nationwide. More troubling, falling is the direct cause of 95% of hip fractures, which lead to death in 20% of cases. More than one-third of older adults hospitalized for a fall are discharged to long-term care facilities instead of returning home.
But here's the good news: most falls are preventable. With the right strategies, seniors can significantly reduce their risk while maintaining the independence they value. This means addressing multiple factors—from physical fitness and medication management to home safety modifications and proper footwear.
For families, the worry is constant. Will Mom be okay at home today? Did Dad take his medications safely? Is their environment secure? Understanding fall prevention isn't just about statistics—it's about giving your loved ones the tools to live confidently and giving you peace of mind.
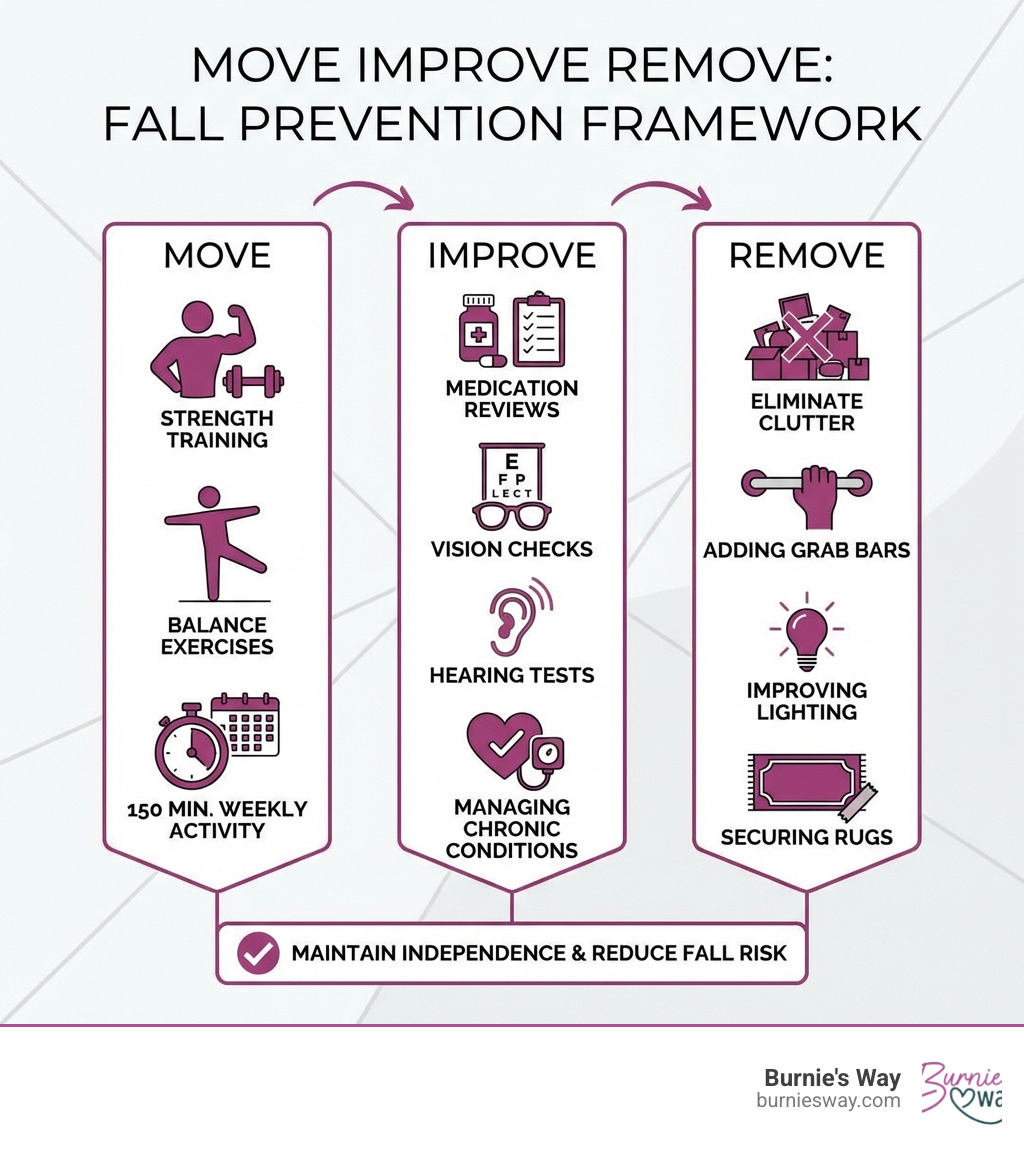
Quick fall prevention seniors terms:
While the statistics mentioned in the introduction highlight a national crisis, the impact on an individual level is even more profound. When we talk about fall prevention seniors, we aren't just talking about avoiding a bruise. We are talking about protecting a person’s ability to drive, visit friends, and enjoy their own home.
In our experience supporting families across Virginia, we’ve seen how a single trip over a loose rug can ripple through a family. Beyond the immediate pain, falls often result in a "fear of falling." This psychological impact is significant; it often leads seniors to limit their activities. When someone stops moving to stay "safe," their muscles weaken, their balance worsens, and ironically, their risk of falling actually increases.
The physical toll is equally staggering. Falling is the leading cause of injury for older adults, resulting in roughly 85% of injury-related hospital admissions for those aged 65 and over. Perhaps most concerning is that 67% of fall victims suffer from life-threatening injuries if they aren’t found within 72 hours. This is why we emphasize not just prevention, but also having a reliable support system in place.

Understanding why falls happen is the first step toward prevention. As we age, our bodies undergo natural changes that can make us less steady on our feet. We often categorize these as biological and behavioral factors:
One of the most overlooked aspects of fall prevention seniors face is the cabinet in their bathroom. As we age, our bodies metabolize medications differently. What worked in our 50s might cause dizziness or confusion in our 70s.
Many common medications—including those for blood pressure, sleep, and even some over-the-counter antihistamines—can cause side effects like drowsiness, blurred vision, or a sudden drop in blood pressure when standing up (postural hypotension).
We always encourage our members to conduct a regular medication review with their doctor or pharmacist at least once a year. This process, sometimes called "deprescribing," involves looking at whether certain medications are still necessary or if dosages need adjustment to reduce the risk of a fall. For more detailed information, you can explore this Medications and Falls Guide.
Maintaining an active lifestyle is perhaps the single most effective way to stay upright. We believe that staying independent starts with staying mobile. The goal isn't necessarily to run a marathon, but to maintain the strength and flexibility needed for daily life.
Current health guidelines suggest that adults aged 65 and older should aim for at least 150 minutes of moderate-intensity physical activity per week. This can be broken down into manageable 10-minute sessions. Crucially, these activities should include balance training at least three days a week.
What we put into our bodies is just as important as how we move them. Proper nutrition supports muscle mass and bone density, which are your internal armor against fall-related injuries.
For more tips on maintaining a balanced diet, you can refer to Healthy Eating for Seniors.
Proactive health management is a cornerstone of fall prevention seniors can rely on. We often help our members coordinate these essential check-ups:
A great way to start is by using the Staying Independent Checklist to identify your personal risk areas.
Did you know that 50% of falls that result in hospitalization happen right at home? Our homes are filled with "invisible" hazards that we’ve lived with for years, but as our mobility changes, these hazards become dangerous.
Creating a safe environment doesn't have to mean turning a house into a hospital. Often, simple elderly home modifications can make a world of difference. We focus on "hazard-proofing" by removing obstacles and adding support where it's needed most.
| Feature | High-Risk (Hazardous) | Low-Risk (Safe) |
|---|---|---|
| Lighting | Dim halls, no night lights | Bright, motion-sensor lights |
| Floors | Loose rugs, cluttered paths | Clear walkways, secured carpets |
| Bathroom | No bars, slippery tub | Grab bars, non-slip mats |
| Stairs | Loose handrails, cluttered steps | Sturdy rails on both sides, clear steps |
| Storage | Items on high shelves | Frequently used items at waist level |
To make your home as safe as possible, we suggest a room-by-room approach:
In Virginia, we have to be particularly mindful of the weather. Rain, ice, and even wet leaves can turn a porch or walkway into a skating rink.
Sometimes, a little extra support is all it takes to maintain total independence. Assistive devices like canes and walkers are not signs of weakness; they are tools for freedom. However, they only work if they are used correctly.
If you use a cane or walker, ensure it is adjusted to the correct height (usually the level of your wrist crease when your arm is hanging down). Check the rubber tips regularly—if they are worn smooth, they won't provide the grip you need.
Personal alarms or emergency response systems are also vital. Since many falls happen when a senior is alone, having a way to call for help instantly provides immense peace of mind for both the senior and their family.
Your shoes are your foundation. Walking around in stocking feet or loose slippers is a major risk factor for slips. We recommend:
Even with the best fall prevention seniors can practice, accidents can happen. Knowing what to do in the moments after a fall can prevent a bad situation from getting worse.
If you fall:
You can watch a step-by-step demonstration in this How to Get Up Safely After a Fall Video. Always tell your doctor about a fall, even if you weren't hurt, as it may be a sign of a new medical issue.
You should have a comprehensive eye exam at least once a year. Vision changes can happen gradually, and staying on top of your prescription ensures you can accurately judge distances and spot hazards in your path.
Tai Chi is often cited as one of the best exercises for balance because it focuses on slow, controlled movements and weight shifting. However, any activity that strengthens your legs and core—such as walking, water aerobics, or simple chair exercises—will significantly help.
Yes. Medications categorized as sedatives, antidepressants, and some blood pressure medications are known to increase fall risk. Even some over-the-counter sleep aids can leave you groggy and unsteady the next morning. Always review your list of medications with a professional annually.
At Burnie's Way, we believe that every senior deserves to live with confidence and joy in their own home. Fall prevention seniors can master isn't just a set of rules; it’s a lifestyle of proactive choices that preserve your freedom.
We understand that managing all these moving parts—coordinating doctor appointments, finding the right home modification experts, and keeping up with exercise routines—can feel overwhelming for families. That is why we are here. Our personalized approach to lifestyle coordination and personal support is designed to handle the "heavy lifting" of daily management, so you can focus on what matters most: spending quality time with your loved ones.
Whether it's helping you organize your home for safety or coordinating a companion to walk with you during your daily exercise, we are committed to your independence. If you're looking for that extra layer of support and peace of mind in Virginia, we invite you to learn more info about our services. Together, we can make "staying safe at home" a reality for years to come.

10 min read
Why Financial Stress Shouldn't Mean Losing Your Independence Bill paying assistance is available through government programs, utility providers, and...

12 min read
Understanding Your Loved One's Right to Refuse Can an elderly person refuse care? Yes. In most situations, a mentally competent adult—regardless of...

13 min read
Why Caregiver Self Care Matters More Than You Think Caregiver self care is the practice of maintaining your own physical, emotional, and mental...