12 min read
Beyond the Basics: A Comprehensive Guide to Eldercare Services
Why Understanding Eldercare Services Matters Now More Than Ever Eldercare services help older adults live safely and independently at home by...
12 min read
 Sydney Giffen
:
March 10, 2026
Sydney Giffen
:
March 10, 2026


Can an elderly person refuse care? Yes. In most situations, a mentally competent adult—regardless of age—has the legal right to refuse support, assistance, or medical treatment, even when family members believe it's needed. This right is rooted in the fundamental principle of personal autonomy: the ability to make one's own decisions about life, body, and daily routines.
Quick Answer:
This doesn't make it any easier when you're watching a parent struggle with tasks that were once simple, or when you're losing sleep over their safety. The conflict between respecting independence and ensuring well-being creates real emotional strain for families.
The truth is that between 70-95% of older adults want to age in place—to stay in their own homes as long as possible. When you suggest help, you may be met with resistance not because they're being difficult, but because they're trying to protect something precious: their sense of self and independence.
This article will help you understand the legal rights your loved one has, why they might be refusing support, and practical strategies for navigating this challenging situation with compassion and respect—while still ensuring their safety and quality of life.
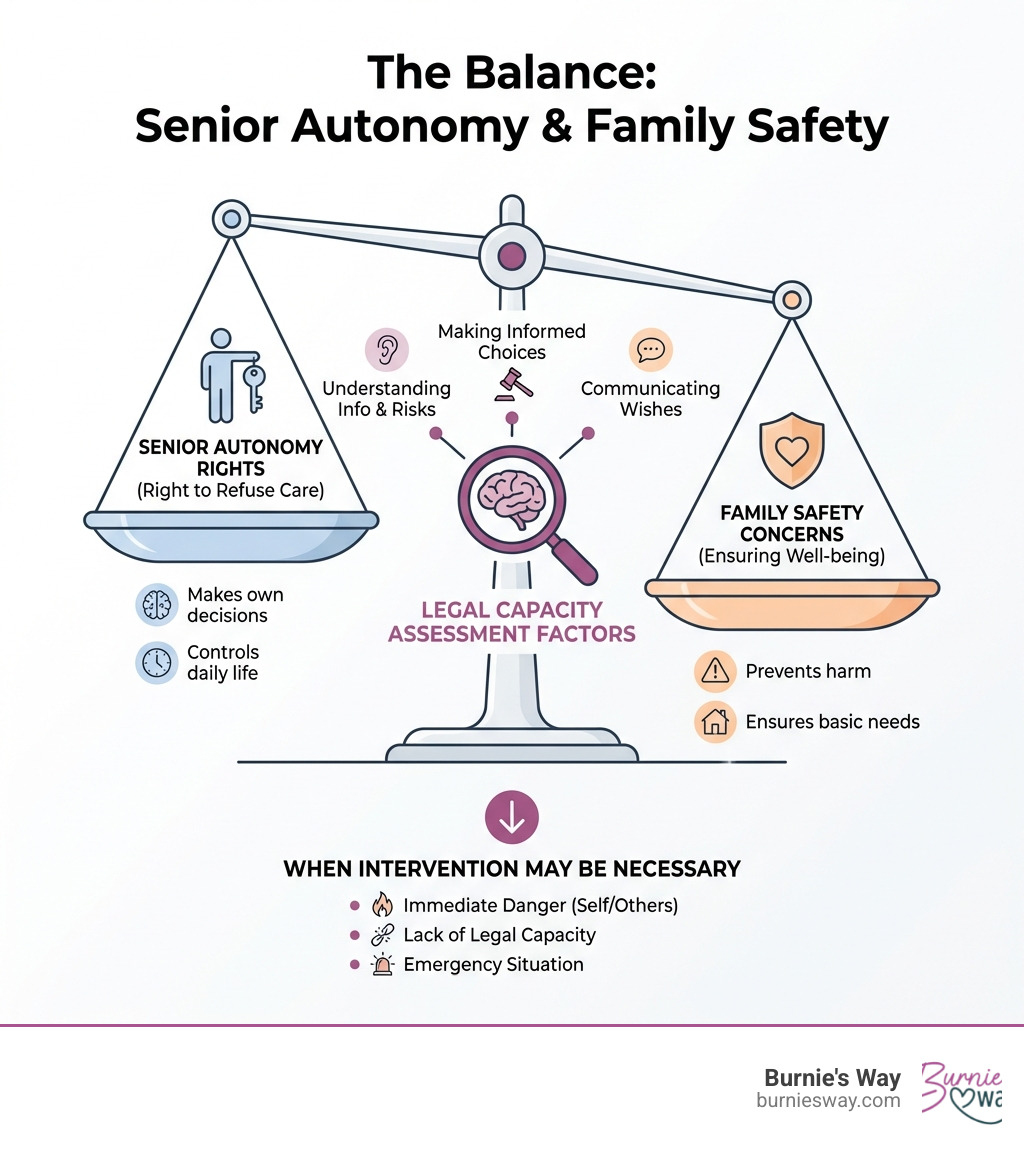
Can an elderly person refuse care helpful reading:
When an elderly loved one refuses help, it's frustrating. We see the need, but from their perspective, the refusal is a complex mix of emotions and fears, not stubbornness. Understanding these underlying reasons is the first step toward finding a solution.

Here are some of the most common reasons why seniors might say "no" to support:
Understanding these reasons helps you approach the conversation with empathy, not frustration. The goal is to address their deeper fears and needs, not to win an argument.
The question "can an elderly person refuse care?" is a legal one, tied to the right of personal autonomy. In the U.S., competent adults can make their own decisions about their lives and personal support, even if others see those choices as "unwise." This right is upheld by the principle of informed consent.
Personal Autonomy: This means individuals have the right to govern their own bodies and lives. For a senior, this includes choosing where to live and what support to accept or decline. As long as they are of sound mind, their choices must be respected.
The Right to Make 'Unwise' Decisions: A competent adult has the right to refuse assistance, even if it leads to negative consequences. If they understand the risks and benefits, their decision stands. While difficult for families to accept, this is a cornerstone of individual liberty.
Informed Consent: For any support, an individual must give informed consent, meaning they must:
The process of obtaining informed consent is central to respecting an individual's autonomy.
Legal Rights: These rights are legally protected. Unless specific legal conditions are met, no one can force a competent elderly person to accept unwanted support.
The Role of Trusted Professionals and Advocates: Involving trusted professionals and advocates—like elder law attorneys or social workers—can be invaluable. They can explain rights, assess situations, and mediate discussions without the emotional weight of family dynamics, ensuring the senior's wishes are understood and respected.
While a competent adult has the right to refuse support, the concept of "competence" hinges on mental capacity. Mental capacity is the ability to make a specific decision at a specific time.
Even with the strong emphasis on autonomy, there are limited circumstances under which an elderly person's refusal of support can be overridden.
Planning ahead with legal documents is one of the most powerful ways to ensure your loved one's wishes are respected, even if their capacity declines.
Here are the key documents we encourage our clients to consider:
Preparing these documents while your loved one is mentally capable prevents future stress and conflict. It allows them to retain control over their future, even if they can't speak for themselves. This foresight is part of How We Work at Burnie's Way, as we help clients plan for future comfort and confidence.
When faced with a loved one refusing support, it's easy to feel helpless or frustrated. But there are compassionate and effective strategies we can employ to steer these difficult conversations and encourage acceptance. Our goal is always to balance their autonomy with their safety and well-being.
Starting the Conversation: The first step is often the hardest. We recommend:
Effective communication is the cornerstone of navigating refusal. We know it’s not always easy, especially with years of family dynamics at play.

Sometimes, a different voice can make all the difference. When your direct appeals aren't working, consider expanding your support network.
Once you understand their reasons for refusal and have opened lines of communication, it's time to explore solutions that address their concerns while still providing necessary support.
Navigating an elderly loved one's refusal of support can bring up many questions. We've gathered some of the most common ones we hear and offer insights to help you through.
Yes, absolutely. This is a fundamental right grounded in personal autonomy. If an elderly person is deemed to have the mental capacity to understand the implications of their decisions—including the risks and benefits of refusing support—their choices must be respected. Even if we, as family members, strongly disagree with their decision and believe it puts them at risk, a competent adult has the legal right to make what others might consider an "unwise" decision. Our role then shifts from trying to persuade them to accepting their choice and finding ways to support them within their chosen boundaries, while ensuring their dignity and safety are still prioritized.
This is a particularly challenging situation because dementia directly impacts mental capacity, which is central to the right to refuse. If your parent has dementia and is refusing help, here's what we suggest:
Contacting Adult Protective Services (APS) is a serious step and should generally be considered a last resort when an elderly person is at significant risk and all other attempts to provide support have failed. You should consider contacting APS if you observe:
APS investigates allegations of abuse, neglect (including self-neglect), and exploitation of vulnerable adults. Their intervention aims to ensure the individual's safety and well-being, which might involve coordinating support services, or in extreme cases, seeking court-ordered guardianship if the individual is deemed incapacitated and at severe risk. APS is there to protect vulnerable adults, and while it's a difficult decision, it's sometimes necessary for their survival.
Navigating the complexities of an elderly loved one's refusal of support is one of the most challenging experiences families face. It's a delicate dance between honoring their autonomy—their fundamental right to make their own choices—and prioritizing their safety and well-being. We understand that this journey is filled with emotional highs and lows, from frustration and fear to deep love and concern.
Our hope is that this guide has provided you with a clearer understanding of why your loved one might be refusing help, what their legal rights are, and practical, empathetic strategies for moving forward. The power of communication, rooted in patience, empathy, and respect, cannot be overstated. By truly listening to their fears, involving trusted individuals, and offering solutions that preserve their independence, we can often find common ground.
At Burnie's Way, we believe in empowering aging adults to live confidently and comfortably in their own homes, on their own terms. We specialize in providing personalized support and coordinating daily life management, acting as a virtual companion and personal assistant. We understand the value of independence and work to improve it, giving families peace of mind.
If you're seeking ways to help your loved one maintain their independence and manage their daily life with dignity, we're here to help. Learn more about how personalized support can help your loved one maintain their independence by exploring Our Services.

12 min read
Why Understanding Eldercare Services Matters Now More Than Ever Eldercare services help older adults live safely and independently at home by...

13 min read
What Continuous Care Services Really Mean for You and Your Family Continuous care services are specialized, short-term support designed to help...

10 min read
Why Elder Care Specialists Matter for Families Today Elder care specialists (also known as Aging Life Care Professionals or Geriatric Care Managers)...